
The Opportunity
Delivering on our mission requires connecting women to medical resources which provide real solutions to real problems.
Infertility
Premenstrual syndrome (PMS)
Ovarian cysts
…
What solutions exist today?
NaProTECHNOLOGY (Natural Procreative Technology) is a women’s health science that monitors and maintains a woman’s reproductive and gynecological health. It provides medical and surgical treatments that cooperate completely with the reproductive system.
Women access these treatments via physicians who are specifically trained in this system.
These physicians interpret a woman's gynecological health through the biomarkers provided by the FertilityCare system.
Women are trained to record these biomarkers from trained FertilityCare practitioners who assist them through managing their gynolocal health during every reproductive stage.
FertilityCare and NaProTECHNOLOGY are only as effective as
1) the quality of care they are able to provide and
2) the number of clients they are able to serve
How do we reach all women?
Reaching all women requires universal access to practitioners and medical professionals. Without practitioners, clients cannot learn the system and connect to medical professionals (where necessary). Without trained medical professionals, clients and Practitioners may identify issues but have no means of addressing them.
Do we have enough researchers to reach all women?
Yes, FertilityCare and NaProTechnology provide a solid foundation that is actively maintained
But…
No recent studies
….
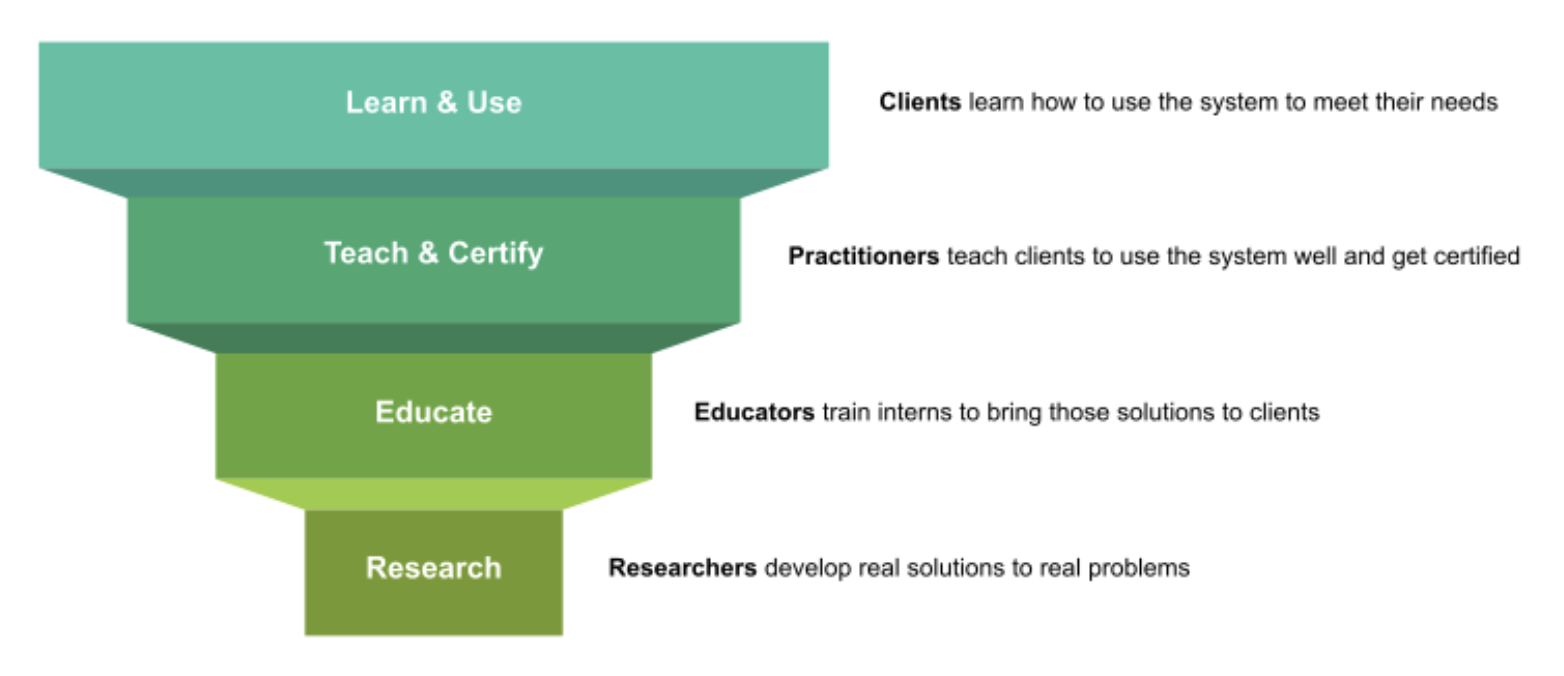
To use the system effectively, clients must learn from qualified practitioners. To become qualified to teach clients, practitioners must learn from education (and ideally become certified). To become qualified to teach practitioners, educators must develop and demonstrate a deep understanding of the research, processes and practices which form the foundation of FertilityCare.
Do we have enough educators to reach all women?
Yes, education programs are regularly held in several continents each year
But…
Not available in all languages
…
Do we have enough practitioners to reach all women?
No, there exist several regions where no fertility care practitioners are available (or available in the client’s language)
…
How do we train and retain more practitioners?
While no formal studies have been conducted on the attrition rates of interns and practitioners, anecdotal evidence suggests that several factors can contribute to interns leaving the education program and practitioners reducing their client load. These factors include:
Time commitments for both seeing clients and processing the follow up paperwork – which is especially heavy during the internship (i.e. MCRs, CRs, etc.)
Time spent on business aspects unrelated to serving clients (i.e. billing, appointment scheduling, branding, marketing, etc.)
. . .
How might we reduce the time spent on these activities and improve not only intern graduation rates, but also the number of clients each can serve without degrading the quality of service?
How do we ensure a high quality of care?
Being able to reach all women is necessary but not sufficient to meet the needs. Growing the number of practitioners without maintaining or improving the quality of care they provide will leave clients with an incomplete grasp of the system and limit their ability to find real solutions to real problems.
How do we ensure all interns receive a comprehensive education?
The current education programs provide a solid foundation which teaches interns the ins and outs of the theory and practice of Fertility Care. This education is backed by rigorous practical phases where interns gain clinical experience working with clients with the support of a supervisor. During this phase of education, the intern gains familiarity with the standard follow up processes, forms and case management scenarios. Unfortunately, breadth and depth of this exposure is limited by the needs of these first 15 clients. If none exhibit a particular case management scenario, the intern may graduate without practical experience managing one or more scenarios.
How might we enable educators to supplement case management practice with scenarios the intern would otherwise not encounter?
How might we enable interns to practice the concepts they learn throughout the education process such as chart correcting, the basics of VDRS, etc.?
How do we ensure all FCPs consistently apply the standard processes?
Learning the system well is only the start. Teaching clients well requires the intern/practitioner to reliably follow the structured follow up process which is supported by the follow up form. Errors in teaching or in documenting observation of how well the client is learning hinders not only the client’s ability to learn the system but also the clinical relevance of the data (silently decreases method effectiveness).
How might we help practitioners identify and correct errors in the follow up form?
